The effects of Covid-19, more widely referred to as coronavirus, are being experienced worldwide, with new cases reported daily.
Today’s declaration by the World Health Organisation of the coronavirus as a pandemic, coupled with the Federal Government’s announcement of targeted funding to both combat the virus and bolster the Australian economy, indicate the real seriousness with which the ongoing coronavirus outbreak should be treated.
Following the death of a 95 year old woman in a Sydney Residential Aged Care Facility (RACF), and the recent diagnosis of two RACF staff members, the aged care industry is preparing itself for the worst, including the very real likelihood of potential lockdowns and quarantines of RACFs occurring.
Infection and Disease Control
The aged care industry is not without experience in situations of this nature, with previous seasons of severe influenza having a profound impact on the response of the industry to infection and disease control in RACF’s. The 2017 influenza outbreak saw aged care providers (Providers) engaged in a national focus on infection controls, with an emphasis on staffing provisions and infection protocols designed to minimise risk of spread.
Just last year RACFs in NSW were placed into lockdown due to the spread of influenza, with Providers experiencing resident deaths, hospitalisation and supply and staffing shortages as a result.
A recent paper released by the Chinese Centre for Disease Control (CCDC) identified the persons with the highest risk of coronavirus related mortality. The below table, sourced from the CCDC paper, identifies the significantly higher risk posed to elderly persons, particularly those within the ages of 70-80+, a trend which may be likely to continue with the international spread of the virus.
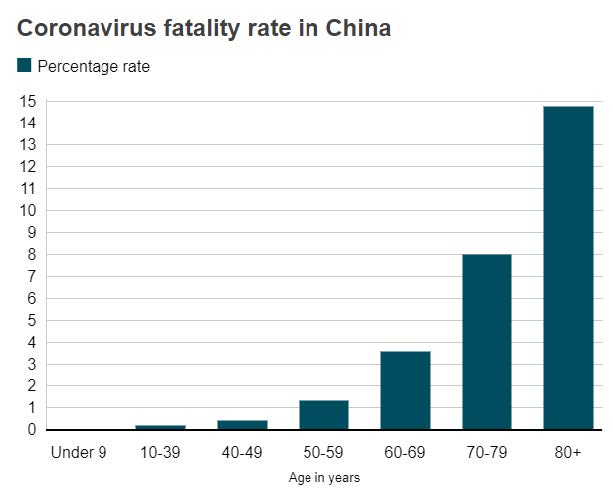
Worryingly, this age demographic is consistent with the typical ages of residents in RACFs.
How Should Providers Respond?
The Aged Care Quality Standards (ACQS) prescribe requirements which are designed to minimise the spread of infection related risks within RACFs. The ACQS Commissioner, Janet Anderson, wrote to all Providers on 2 March 2020, encouraging self-assessments against the ACQS in order to ensure the highest possible compliance with the national guidelines.
Providers are advised that they should:
- Undertake assessments and management of risk associated with infectious outbreaks, if risk is suspected or identified;
- Ensure adequate care of individuals who may be infected;
- Implement protection measures for staff external parties; and
- Notify and communicate with staff, residents and their families and the relevant authorities.
Practical Implications for Providers
As advised, Providers should conduct a self-assessment and review of current infection control protocols in order to determine their suitability to minimise the risk to RACFs and care recipients.
It seems that the ACQS Commission will continue to monitor the situation closely, and in turn, may impose higher standards relating to infection control in response to any increase in risk, such as restrictions to visitation from families, health providers, medical practitioners and third party suppliers.
Providers should begin to prepare staff and residents for potential restrictions and quarantines of RACFs, be it part of the facility, or the facility as a whole, ensuring staff and residents are aware of all processes and procedures to minimise risk to residents, staff and any other external parties. Providers should also prepare for the possibility that staff themselves may be quarantined and should therefore have appropriate staffing contingency plans in place.
For further information or advice, please contact John Fairgray, jfairgray@bbwlaw.com.au, Balveen Saini, bsaini@bbwlaw.com.au, or Josh Mizzi, jmizzi@bbwlaw.com.au.